Ptosis refers to a vertical narrowing of the palpebral fissure secondary to drooping of the upper eyelid to a lower than normal position. Multiple surgical procedures can be used to correct ptosis including, frontalis sling, levator advancement, Fasanella Servat operation, and Mullerectomy. The selection of one technique over another depends on the consideration of several factors including the degree of ptosis, the degree of levator muscle function as well as the surgeon experience. Detailed examination and accurate measurements help to decide the procedure that may be required in each patient.
When to treat
The primary indications for treatment of congenital ptosis are amblyopia and abnormal head positioning. In the setting of severe unilateral ptosis, stimulus deprivation amblyopia is imminent and early surgery is advised and routinely performed at preschool age. Severe bilateral (or unilateral) ptosis can cause a patient to assume an obvious chin-up head position that can interfere with the child's normal functioning. If neither of these two issues is at play, the correction of ptosis can be delayed until the patient is old enough to have the surgery performed with only local anesthesia, as this makes intraoperative adjustments possible.
If a patient with ptosis also requires strabismus surgery, operating on the vertical muscles can alter the eyelid position. Therefore, ptosis surgery is often deferred until after the strabismus has been corrected.
Acquired aponeurotic ptosis that causes significant superior visual field loss or difficulty with reading is considered to be afunctionalproblem, and correction of ptosis often improves the patient’s ability to perform daily activities. In many instances, ptosis is considered to be acosmeticproblem, causing a tired or sleepy appearance in the absence of a visual function deficit.
|
Sr No |
Indication |
|
1 |
Amblyopia |
|
2 |
Abnormal Head posture |
|
3 |
Superior visual field obstruction |
|
4 |
Cosmetic correction |
Table 1: Indications for surgery
How to treat
The amount of ptosis (determined by MRD1) and degree of levator function are the two most important measurements while deciding the surgical plan; other important findings include – bell’s phenomenon and corneal sensations. In patients with good levator function, surgical correction is generally directed towards advancing or reattaching the levator aponeurosis. However, if levator function is poor or absent, frontalis muscle suspension techniques are preferred. The surgeon’s comfort level and experience with various procedures is also an important factor. For mild to moderated degrees of ptosis, a fasanella servat or mullers muscle resection may be performed.
MULLER’S MUSCLE CONJUNCTIVAL RESECTION (MMCR)
The Muller's muscle is an involuntary, sympathetically innervated muscle that originates below the levator aponeurosis just distal to the Whitnall's ligament. It attaches to the superior tarsal border by a small tendon and is responsible for an estimated 2–3 mm of eyelid elevation. This particular procedure is recommended for patients who respond well to the phenylephrine test, thereby shortening a responsive Muller's muscle.
It was originally described as a modification of the Fasanella-Servat procedure, which involves the excision of 3mm of tarsus. MMCR is a posterior eyelid ptosis repair technique, which spares the tarsus. The obvious advantage of this modification is that the tarsus and the meibomian glands remain undisturbed. Although various authors have given their formulae for the amount of resection, Putterman’s techniques are the most practiced: 8.5mm resection if 10% phenylephrine raises the lid to exactly where you want it, adding or subtracting 1mm of resection for every 0.5mm of desired increased or decreased lid height desired, up to a range of 6.5mm to 9.5mm. Since it is a posterior approach and leaves no visible scar, MMCR is a great option in patients without excess upper eyelid skin. In elderly patients with significant dermatochalasis, an upper eyelid blepharoplasty may be combined with this procedure.
LEVATOR SURGERY – RESECTION / REATTACHMENT / ADVANCEMENT
Resection and advancement of the levator aponeurosis is a technique often used in the correction of ptosis in patients with greater than 5 mm of levator function. This technique is routinely performed via the exposure of the levator aponeurosis through an upper eyelid crease incision (anterior approach), then advancing the levator aponeurosis by folding or excising the muscle and reattaching the aponeurosis to the anterior surface of the tarsus.
In patients with aponeurotic ptosis, with dehiscence of the levator aponeurosis from its tarsal attachment, a mere reattachment or advancement with non-absorbable or permanent sutures may be needed. This is done under local anesthesia and the final eyelid position can be adjusted on the table.
Unlike levator surgery in adults, the amount of resection cannot be adjusted intraoperatively in children and needs to be decided preoperatively. Another difference between adult and pediatric levator resections is that children with congenital ptosis generally require a much larger levator advancement. Most levator resections in children require a dissection superior to Whitnall's ligament except in the mildest of cases, but this is rarely necessary when correcting adult involutional ptosis.
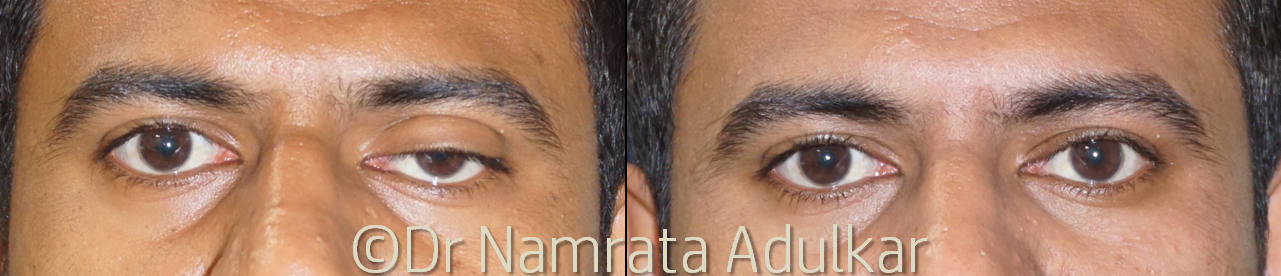
Figure 1: Before and after photographs of a 27 years young man who underwent left eye levator resection under local anesthesia.
There are numerous ways to estimate the amount of levator resection necessary to correct congenital ptosis. The two methods that are most commonly cited and used are those explained by Beard and Berke in their respective reports of congenital ptosis repair.
The method explained by Beard incorporates both eyelid excursion and amount of ptosis to estimate the amount of levator to be resected. Please see Table 2 for the specific figures for this estimation
|
Amount of Ptosis |
Upper eyelid excursion |
Amount of Resection |
|
0-5 mm (poor) |
22-27 mm |
|
|
2 mm (mild) |
6-11 mm (fair) |
16-21 mm |
|
12 or more (good) |
10-15 mm |
|
|
0-5 mm (poor) |
Maximum (30 mm) |
|
|
3 mm (moderate) |
6-11 mm (fair) |
22-27 mm |
|
12 or more (good) |
16-21 mm |
|
|
0-5 mm (poor) |
Maximum (30 mm) |
|
|
4 mm or more (severe) |
6-11 mm (fair) |
25-30 mm |
|
12 or more (good) |
25-30 mm |
|
Table 2:Estimation of Levator resection (Beard, 1976)
The method described by Berke uses an upper eyelid excursion not to determine the amount of levator that needs to be resected, but rather to determine the intraoperative eyelid height at the end of the surgery. The idea behind this approach is that an eyelid with good excursion will rise from its final intraoperative height, and an eyelid with poor excursion may drop from its final intraoperative position.
|
Upper eyelid excursion |
Superior corneal coverage by the upper eyelid |
|
0-5 mm (poor) |
0 mm (lid margin at superior limbus) |
|
6-11 (fair) |
2 mm |
|
12 or more (good) |
4 mm |
Table 3:Intraoperative eyelid height (Berke 1959 and Berke1961)
WHITNALL’S SLING
The Whitnall sling procedure involves maximal levator resection (>25mm), up to Whitnall’s ligament, combined with suturing of the superior tarsal edge to Whitnall’s ligament with either absorbable or non-absorbable sutures. It can be used in cases of moderate to severe ptosis with poor to fair levator function. A superior tarsectomy can be performed as well, with an estimated 1 to 1.5 mm of additional lid elevation expected from a 5-mm resection.However, patients with maximal or supermaximal levator resection commonly have significant lagophthalmos in the immediate postoperative period and must be counselled on frequent lubrication.
TARSOFRONTAL SLING OR FRONTALIS SUSPENSION
Frontalis sling is one of the most commonly used operations for ptosis with poor levator function. In this procedure, the upper lid is linked to the frontalis, such that contracting the frontalis will simultaneously elevate the lid. There are multiple variations in technique. The sling can be placed in a pentagon (See Figure 2), single-triangle, or double-triangle configuration via supraciliary stab incision or lid crease incision.
|
Severe congenital ptosis with poor levator function (<4mm) |
|
Marcus Gunn Jaw Winking ptosis |
|
Traumatic ptosis with poor levator function |
|
Third nerve palsy |
|
CPEO |
|
Myasthenia |
Table 4: Indications of Tarsofrontal Sling
Different materials have been used for suspension, including autogenous or banked fascia lata; alloplastic materials like silicone rods; polyester; silk; stainless steel; monofilament nylon; polytetrafluoroethylene; and polypropylene.Some surgeons consider autogenous fascia lata the best material, due to its biocompatibility and longevity, although it requires a second surgical site and patients must be at least 3 years old to provide a graft of adequate length.Silicone rods are one of the most frequently used alloplastic materials as their elastic nature allows both good eyelid height and complete eyelid closure.
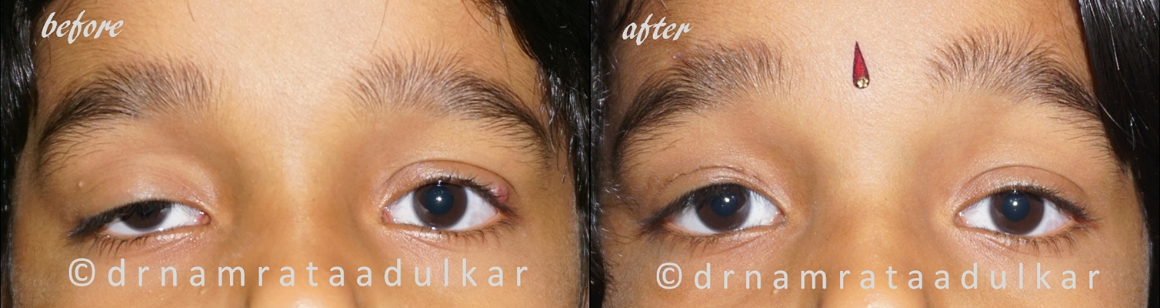
Figure 2: Before and after photographs of a 6 years young child who underwent right upper eyelid frontalis suspension with silicon rod.
Disadvantages of this procedure include the risk of lagophthalmos and eyelid lag in downgaze. There is a risk of infection, inflammation, granuloma formation, and extrusion with the use of alloplastic materials like silicone. There may be cosmetic considerations that include scarring in young children, unsatisfactory geometric tenting of the pretarsal and preseptal skin, loss of the eyelid crease, and a poor tarso-corneal interface seen upon brow elevation and down-gaze.Over time the sling does come down and ptosis may recur in about one-fourth of patients at 2 years.
FRONTALIS MUSCLE FLAP
The frontalis muscle flap procedure has evolved from the frontalis sling and is recommended for use in cases of severe ptosis with levator function less than 4 mm. It involves elevating the innervated frontalis muscle flap, passing it over a pulley created near the insertion of the orbital septum at the superior orbital rim, which redirects the pull of the frontalis to elevate the lid, and then attaching the frontalis muscle to the tarsal plate. It eliminates the need for alloplastic or autologous sling for frontalis suspension to the eyelid as well as improving the direction of the pull.In addition, there is minimal ptosis on upward gaze, less lid lag on downward gaze, preservation of eyelid contour, and reduced tendency for the eyelid to pull away from the eye. Complications of frontalis muscle flap include transient postoperative forehead anesthesia with spontaneous recovery, eyebrow asymmetry, reduced eyelid excursion with an extreme upward and downward gaze, lagophthalmos, and overcorrection possibly due to the frontalis muscle being stronger than the levator muscle.
Because ptosis repair is an elective surgical procedure, it is particularly important for the surgeon to have a preoperative discussion with the patient to communicate the alternatives, potential risks, and benefits.
References
- Allard FD, Durairaj VD. Current techniques in surgical correction of congenital ptosis.Middle East Afr J Ophthalmol. 2010;17(2):129-133.
- Putterman AM, Urist MJ. Müller’s muscle-conjunctival resection. Arch Ophthalmol. 1975;93(8):619-623.
- Putterman AM, Fett DR. Müller’s muscle in the treatment of upper eyelid ptosis: a ten-year study. Ophthalmic Surg. 1986;17(6):354-360.
- Hatt M, Anderson RL. Ptosis surgery: Anterior approach for levator aponeurosis shortening.Ophthalmologica.1979;179:94–8.
- Berke RN. Results of resection of the levator muscle in congenital ptosis. Arch Ophthalmol 1959;62:177.
- Beard C, Sullivan JH. Ptosis. Current Concepts. Int Ophthalmol Clin 1978; 18:53-73
- Jordan DR, Anderson RL. The aponeurotic approach to congenital ptosis.Ophthalmic Surg.1990;21:237–44.
- Anderson RL, Jordan DR, Dutton JJ. Whitnall's sling for poor function ptosis.Arch Ophthalmol.1990;108:1628–32.
- Ben Simon GJ, Macedo AA, Schwarcz RM, Wang DY, McCann JD, Goldberg RA. Frontalis suspension for upper eyelid ptosis: Evaluation of different surgical designs and suture material.Am J Ophthalmol.2005;140:877–85.
- Betharia SM. Frontalis sling: A modified simple technique.Br J Ophthalmol.1985;69:443–5.
- Ramirez OM, Pena G. Frontalis muscle advancement: A dynamic structure for the treatment of severe congenital eyelid ptosis.Plast Reconstr Surg.2004;113:1841–9.discussion 1850–1.
- Holds JB, McLeish WM, Anderson RL. Whitnall's sling with superior tarsectomy for the correction of severe unilateral blepharoptosis.Arch Ophthalmol.1993;111:1285–91.
- Goldey SH, Baylis HI, Goldberg RA, Shorr N. Frontalis muscle flap advancement for correction of blepharoptosis.Ophthal Plast Reconstr Surg.2000;16:83–93.
